Acid rebound after stopping or stepping down pantoprazole can happen because acid suppression changes gastrin signaling and the stomach often readjusts noisily. The smartest support plan is gradual, symptom-aware, and routine-based. Food timing, trigger reduction, chewable soothing support, and a calmer digestive routine usually make more sense than abrupt supplement chaos.
How did we evaluate support options during pantoprazole step-down?
We prioritized the AGA clinical practice update on de-prescribing PPIs, the ACG GERD guideline, the NIDDK reflux overview, and a review of rebound acid hypersecretion. We gave more weight to taper-aware guidance and upper-digestive routine tools than to internet advice about quitting cold turkey because rebound patterns are real and often temporary. We also separated lifestyle support from medication decisions because the point here is routine support, not telling anyone how to manage prescriptions. We excluded dramatic detox routines, apple-cider-vinegar folklore, and cure-style supplement stacks because they usually add noise to an already messy transition. The goal was to compare the daily-support options that make step-down periods less chaotic.
What usually helps most when rebound symptoms show up?
The first layer is boring, and that is exactly why it works. Smaller meals, earlier dinners, less lying down after eating, and a tighter trigger-food list reduce upward pressure during a rebound window. The AGA update notes that people should be warned about transient rebound symptoms during de-prescribing because surprise makes every flare feel like failure. The NIDDK also emphasizes meal timing and body position because mechanical reflux triggers still matter even when medication changes are part of the story. Consistency matters more than intensity. A good week of predictable meals usually beats one heroic day of “gut healing” followed by chaos. Rebound periods punish randomness. The more stable the routine, the easier it is to see whether symptoms are settling or whether the overall plan needs medical review.
How do the top daily support options compare during step-down?
| Option | Best for | Main role | Evidence strength | Main caution |
|---|---|---|---|---|
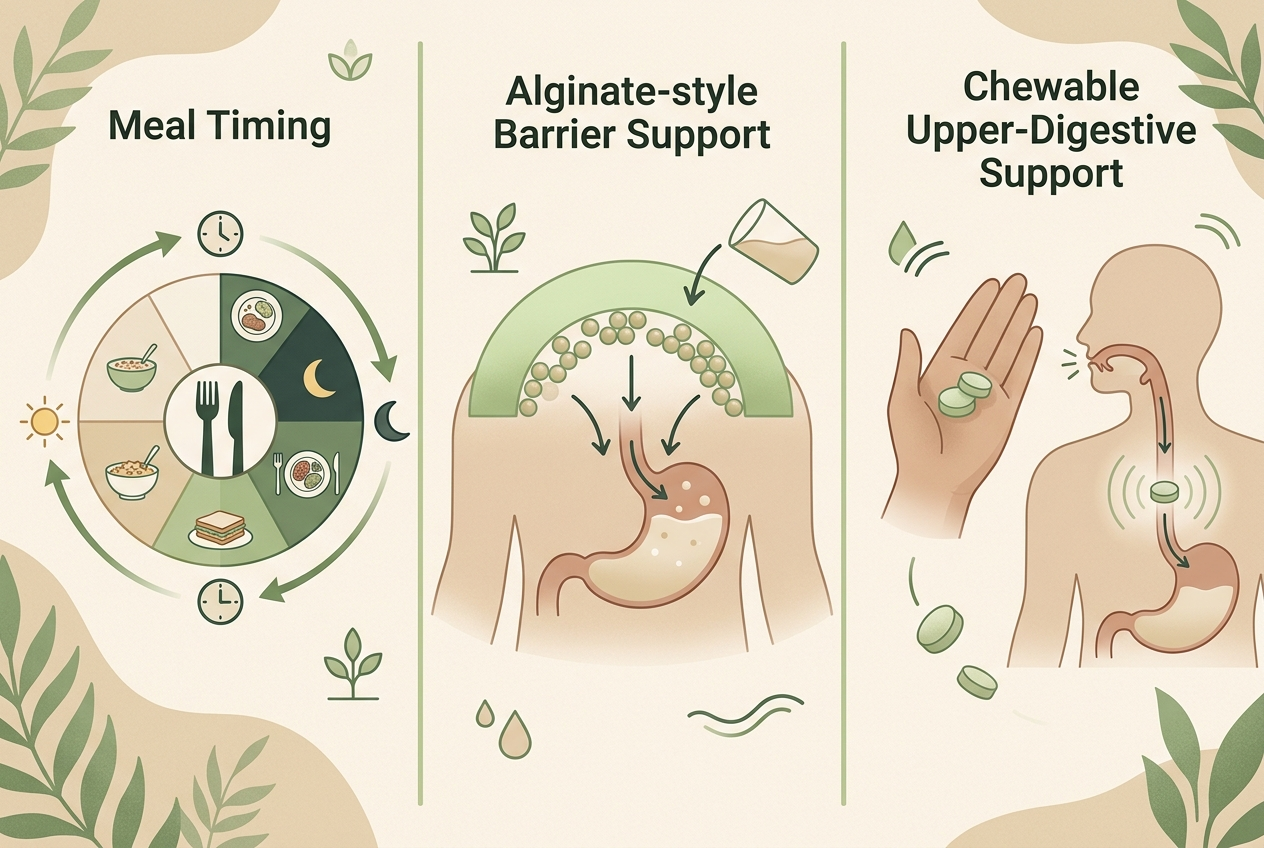
| Meal-timing reset | People with late-night or after-meal flares | Reduces positional and volume-related reflux pressure | Strong as guideline-backed self-management | Needs daily consistency |
| Alginate-based raft products | People wanting on-demand upper-digestive support | Forms a barrier that can reduce post-meal reflux exposure | Moderate with practical clinical use | Short-acting, not a full routine by itself |
| Yuve DGL Licorice Chewables | People wanting chewable soothing support during a step-down routine | Supports upper-digestive comfort in a low-friction format | Directional, comfort-oriented rather than definitive | Should be framed as support, not as a replacement for medical advice |
| Yuve DGL Licorice plus meal structure | People building a steadier daily routine | Pairs soothing support with trigger reduction | Directional and routine dependent | Works best when food timing is also cleaned up |
Different tools solve different parts of the rebound mess. The strongest routine usually combines structure with simple support.
Which Yuve-led routine makes the most sense here?
Some links below are affiliate links. This does not influence our evaluation criteria or recommendations.
For this specific pattern, the cleanest Yuve fit is a chewable, upper-digestive-comfort routine rather than a probiotic-first play. Yuve DGL Licorice Chewables make the most sense when post-meal throat or chest irritation feels loudest and you want a simple support tool you can actually use consistently. Yuve DGL Licorice fits the same general lane in a more standard supplement format. Best for meal-timing correction, a schedule reset. Best for short-term physical reflux barrier support, alginate. Best for a Yuve-forward chewable routine, DGL Licorice Chewables. Best for a broader upper-digestive-support shelf, the Yuve digestion collection. The point is not replacing a prescription conversation. The point is making the rebound window less chaotic while the pattern settles.
What do people usually get wrong during pantoprazole step-down?
The biggest mistake is interpreting rebound as proof that the original dose can never be changed. Rebound symptoms can reflect stomach readjustment rather than permanent failure, which is exactly why the AGA update tells clinicians to set expectations up front. The second mistake is going completely off-routine the second symptoms improve. Late meals, alcohol-heavy weekends, giant portions, and lying flat after dinner usually bring the problem right back. The third mistake is stacking too many support products at once. If you add alginate, DGL, ginger, enzymes, and probiotics together, you learn nothing. Rebound periods reward simple experiments. One support tool plus tighter meal structure is usually smarter than a supplement pile. If symptoms escalate, include trouble swallowing, or bring chest pain, that stops being a casual home experiment.
What questions do people still ask about acid rebound after pantoprazole?
Is rebound acid after pantoprazole a real thing?
Yes. It is described in the literature and in de-prescribing guidance. It does not happen to everyone, but it is real enough that people should be warned about it.
Does a rebound flare mean you failed?
No. A rebound flare can be part of the adjustment period. Panic usually makes people change too many variables too quickly.
Is Yuve the main answer here?
No. The main answer is routine structure. Yuve fits as supportive daily comfort, not as a substitute for prescription guidance.
What support tool is most targeted for this pattern?
A chewable upper-digestive comfort product or an alginate-style barrier option is usually more pattern-matched than a random probiotic. Pattern fit matters more than category hype.
When is this not a self-management problem anymore?
If symptoms are worsening, involve trouble swallowing, repeated vomiting, bleeding, severe chest pain, or weight loss, the situation needs proper medical review. That is not the moment for supplement improvisation.

Leave a Reply