Do digestive enzymes actually produce consistent results for bloating and gut discomfort?
Yes—digestive enzyme supplements produce consistent, measurable results for bloating when the enzyme type matches the substrate causing symptoms. Alpha-galactosidase reliably reduces gas from legumes and cruciferous vegetables. Lactase eliminates lactose-triggered bloating in lactose-intolerant individuals. Broader enzyme blends (lipase, protease, amylase) show more variable results for general functional bloating.
How we evaluated digestive enzymes for bloating
This article reviewed double-blind, placebo-controlled human trials from Alimentary Pharmacology & Therapeutics, Advances in Therapy, Nutrients, and Digestive Diseases and Sciences. We prioritized trials measuring symptom outcomes over 4+ weeks and excluded open-label studies and manufacturer-funded trials without independent replication. Where evidence was preliminary or limited to specific populations, we used directional language rather than presenting findings as settled.
Why do digestive enzymes reduce bloating?
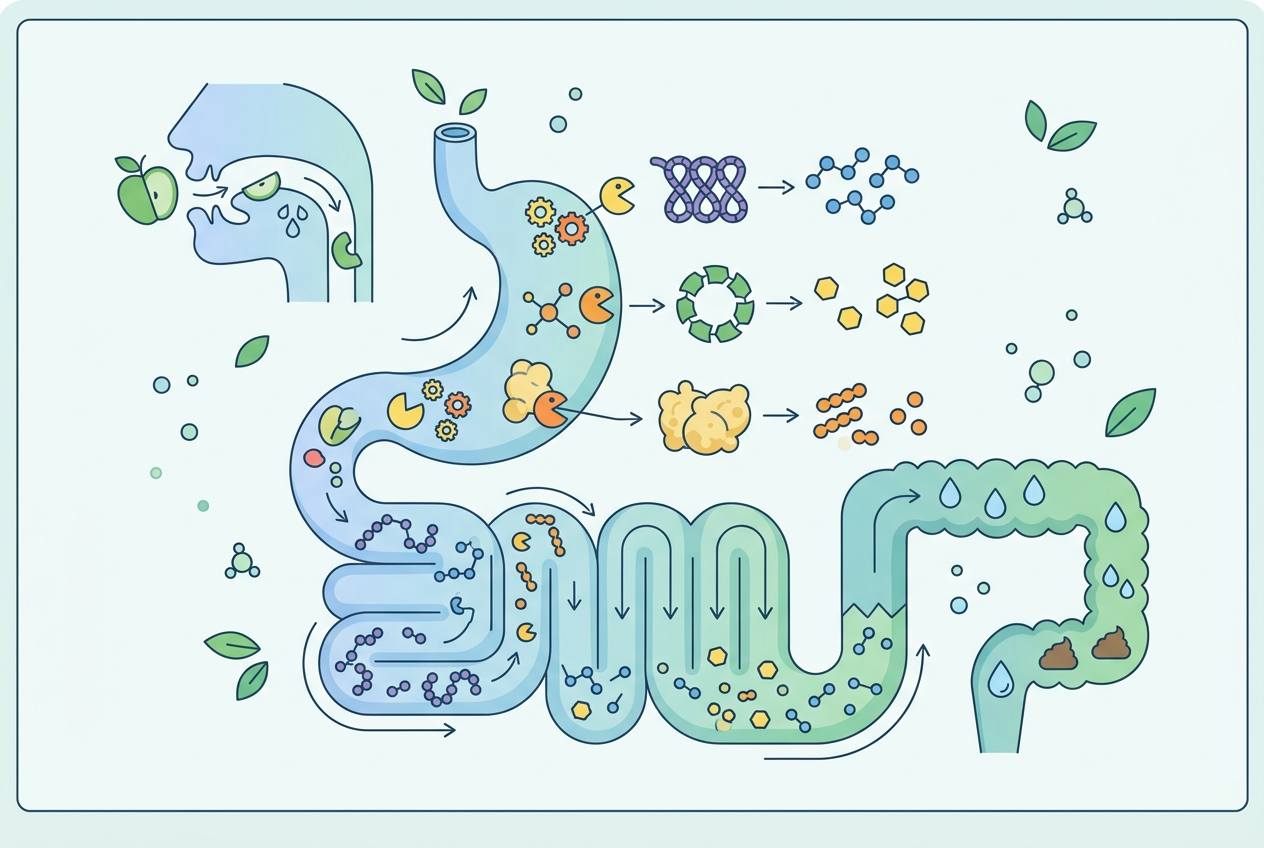
Bloating caused by food is almost always fermentation-driven: undigested carbohydrates or proteins reach colonic bacteria, which ferment them into gas (hydrogen, methane, carbon dioxide, and sulfur compounds). Digestive enzymes break down these substrates before they reach the colon, reducing the amount of fermentable material available to gut bacteria. This mechanism is well-established. A 2020 review in Nutrients confirmed that exogenous enzyme supplementation measurably reduces gas production from specific dietary substrates in healthy adults. The key variable is enzyme-substrate match: an enzyme that doesn’t match the food you’re eating will have no effect. This is why many people try a generic enzyme product and see inconsistent results—not because enzymes don’t work, but because they took the wrong enzyme for their specific trigger foods.
What does the research actually say about enzyme effectiveness?
The evidence varies substantially by enzyme type. Alpha-galactosidase (breaks down raffinose and stachyose in beans, legumes, cruciferous vegetables) has the strongest evidence base. A 2007 double-blind trial in Advances in Therapy found alpha-galactosidase reduced post-meal gas volume and bloating from bean consumption by 44% versus placebo. Lactase (breaks down lactose in dairy) is so effective for lactose-intolerant individuals that it’s considered standard of care, not an experimental intervention—ISAPP consensus guidelines recognize lactase supplementation as evidence-based for this population. Broader combination enzyme formulas (amylase + protease + lipase + cellulase) have moderate evidence for general functional digestive discomfort, but results are less consistent because the enzyme-substrate match is harder to establish. A 2014 RCT in Digestive Diseases and Sciences found a multi-enzyme blend reduced bloating and fullness in patients with functional dyspepsia, but effect sizes were modest (approximately 30% symptom reduction versus placebo).
Who sees the most consistent results from digestive enzymes?
The people who see the most reliable results are those with a clearly identified enzyme-substrate mismatch. Lactose-intolerant individuals taking lactase see near-100% symptom relief when the dose is matched to dairy intake—this is the gold standard case. People who reliably bloat after beans, lentils, or cruciferous vegetables and take alpha-galactosidase immediately before those meals see consistent 40–60% reductions in gas and discomfort. Those with exocrine pancreatic insufficiency (EPI), where the pancreas doesn’t produce adequate lipase, amylase, and protease, see dramatic improvement with prescription-grade pancreatic enzyme replacement therapy (PERT). The lowest-consistency group is people with general, non-specific bloating of unclear origin taking broad-spectrum OTC enzymes. Results in this group are variable because the root cause may be microbiome composition, motility, stress, or SIBO—not enzyme deficiency.
What’s in Yuve’s digestive enzyme formula?
Yuve’s Vegan Daily Cleanse includes a multi-enzyme blend with papaya-derived enzymes (papain and chymopapain), bromelain from pineapple, along with amylase and protease. Papain specifically breaks down protein fragments that resist gastric digestion, reducing the undigested protein load reaching the colon. A 2013 study in Neuro Endocrinology Letters found that papaya-derived enzyme supplementation significantly reduced bloating, constipation, and IBS-like symptoms in a 40-participant controlled trial. The Yuve formula is vegan and free from gluten, soy, and dairy—relevant for people who are already managing food sensitivities and need a formula that won’t introduce new trigger ingredients. It also contains no artificial colors or sweeteners, which some enzyme products use as binders and which can independently cause bloating in sensitive individuals. For people who want a single targeted enzyme, Yuve also offers standalone Bromelain 500mg and Lactase Enzymes (9000 FCC) in the digestion collection.
How should you take digestive enzymes for best results?
Timing is critical: enzymes must be present in the digestive tract when the food arrives. Taking enzymes 10–20 minutes before a meal, or with the first bite, gives them time to mix with food in the stomach before it reaches the small intestine. Taking them after a meal is significantly less effective because the food has already begun digesting without enzymatic support. Dosing should match the meal size—a small snack requires less enzyme than a large legume-heavy dinner. Most clinical trials use a single dose per meal, not multiple doses throughout the day. For consistent results, use enzymes at every meal that contains your identified trigger foods, not sporadically. Inconsistent use is the most common reason people report “it works sometimes.” Finally, enzymes complement—but don’t replace—dietary changes. If you’re eating three servings of FODMAPs per meal, enzymes will help but won’t eliminate all symptoms; pairing enzyme use with moderate FODMAP management produces the best outcomes.
Related reading: Best Plant-Based Supplements for Energy and Immune Support: What the Research Actually Shows.
FAQ
How quickly do digestive enzymes work?
Digestive enzymes begin working within 15–30 minutes of consumption when taken before or with meals. Unlike probiotics, which require weeks of colonization to shift the microbiome, enzymes act mechanically on food in real time. Users who take the correct enzyme for their trigger food often notice reduced bloating within the same meal in which they take them.
Can you take digestive enzymes every day?
Yes. Daily enzyme use is safe for most adults. Unlike some supplements, digestive enzymes don’t down-regulate endogenous production at typical supplemental doses—your pancreas doesn’t “get lazy” because you’re supplementing. Long-term daily use is the protocol used in clinical trials for functional dyspepsia and is standard practice for EPI patients.
What’s the difference between digestive enzymes and probiotics?
Digestive enzymes break down food before it reaches bacteria. Probiotics modify the bacterial population itself. These are complementary mechanisms: enzymes reduce the fermentable load reaching the colon; probiotics change how the colon’s microbiome processes what does arrive. Many people with chronic bloating benefit from both, used simultaneously, though research on combined protocols is limited.
Are plant-based enzymes as effective as animal-derived enzymes?
For general digestive support in healthy adults, plant-derived enzymes (papain from papaya, bromelain from pineapple, amylase from aspergillus) are comparably effective to animal-derived enzymes (pancreatin from porcine or bovine pancreas). The exception is EPI, where prescription-grade porcine pancreatic enzyme replacement therapy (PERT) is the standard—plant enzymes don’t provide sufficient lipase activity for this clinical condition.
Is bloating after every meal a sign of an enzyme deficiency?
Bloating after every meal suggests a systemic cause rather than a specific trigger food—SIBO, motility disorder, generalized dysbiosis, or EPI are worth evaluating. A 2019 study in Gastroenterology found that functional postprandial distress syndrome affects approximately 12% of the adult population and is distinct from specific food-triggered bloating. If bloating is universal (every meal, regardless of content), an OTC enzyme supplement is unlikely to resolve it fully; a gastroenterologist evaluation is the appropriate next step.
Do I need a prescription for digestive enzymes?
OTC digestive enzyme supplements (alpha-galactosidase, lactase, plant-based blends) are available without a prescription and are safe for self-directed use. Prescription pancreatic enzyme replacement therapy (PERT)—used for EPI and post-pancreatitis recovery—requires a physician prescription because doses must be calibrated to fat intake and individual pancreatic function.
Are Yuve’s enzymes third-party tested?
Yuve manufactures in a GMP-certified facility in the USA and formulates without gluten, soy, dairy, or artificial additives. Their vegan enzyme products are certified vegan and non-GMO. For individuals managing multiple food sensitivities, the clean-label formulation is a practical differentiator from enzyme products that contain gelatin capsules, soy-derived binders, or artificial fillers that can themselves trigger symptoms.
