People have tried the blood type diet for reflux, but the evidence does not support ABO blood type as a reliable way to choose reflux-friendly foods. Pattern tracking, clinician-guided trigger review, and a consistent digestive routine have better rationale. Use blood type rules as a personal experiment only if they do not replace medical guidance.
How did we evaluate the blood type diet for reflux-related digestive comfort?
This review evaluated ABO blood type dieting against three criteria: direct reflux evidence, practical trigger identification, and everyday digestive routine fit. PubMed-indexed human research, gastroenterology guidance, and National Institute of Diabetes and Digestive and Kidney Diseases patient guidance received more weight than testimonials, Reddit anecdotes, or diet-book rules. Evidence that addressed ABO blood type and diet outcomes counted as relevant; evidence that only discussed general restriction, weight change, or food avoidance counted as indirect. This review excluded claims that a supplement, diet, or food pattern can diagnose, treat, cure, or prevent reflux disease, because the safer question is whether a routine supports digestive comfort while a clinician handles persistent symptoms. Product fit was judged by whether the routine could be repeated daily, explained plainly, and described without disease-treatment language or unsupported promises in practice.
Does the blood type diet have evidence for reflux-related symptoms?
The blood type diet does not have good evidence as a reflux-specific food strategy. A systematic review in the American Journal of Clinical Nutrition found no eligible studies proving health benefits from blood type diets, and a later PLOS ONE analysis found that cardiometabolic changes were not explained by ABO genotype. That matters for reflux-related comfort because the diet assigns broad rules to type O, A, B, and AB instead of testing a person’s actual response to coffee, alcohol, late meals, high-fat meals, peppermint, chocolate, citrus, tomato, or portion size. Blood type rules can still change behavior because they reduce foods and add structure. That does not make ABO status the active mechanism. A person who feels better after the diet may be responding to fewer personal triggers, smaller meals, lower alcohol intake, or better meal timing rather than blood type matching.
What should you try instead of matching meals to ABO blood type?
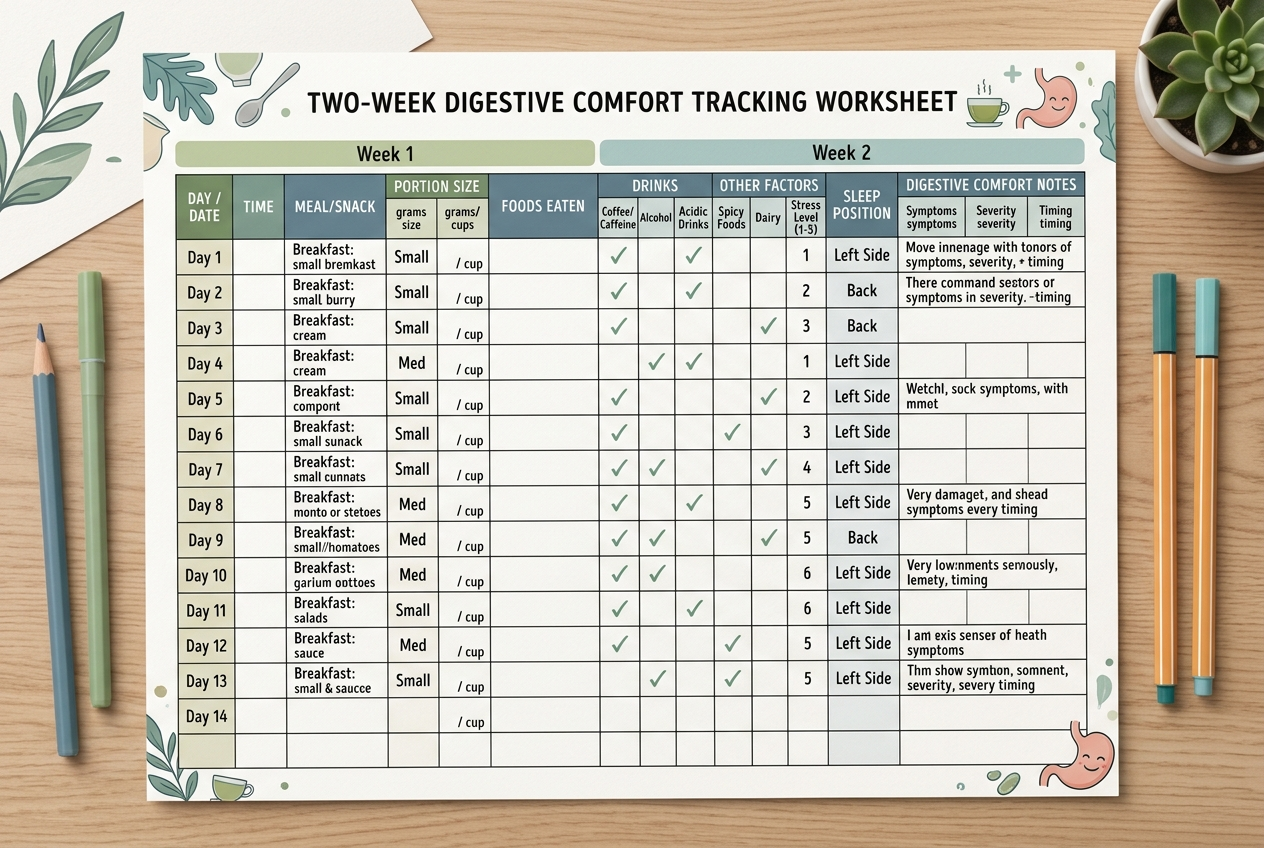
A better first experiment is reflux-pattern tracking, because the person, meal, timing, posture, stress, alcohol, caffeine, and portion size are the variables that actually change day to day. The NIDDK lists high-fat foods, chocolate, coffee, peppermint, spicy foods, acidic foods, and alcoholic drinks as common items some people may need to limit, but it does not say every person must avoid every item forever. A two-week log gives cleaner information than an ABO food list because it links a specific meal pattern to a specific comfort outcome. Track meal time, meal size, food categories, symptoms, sleep position, and supplement timing. If symptoms are frequent, severe, new, or paired with trouble swallowing, unexplained weight loss, bleeding, or chest pain, medical evaluation should replace self-experimenting. Tracking is a decision tool, not a diagnosis or medical care.
How do the common options compare for reflux-related digestive comfort?
Blood type dieting, reflux-pattern tracking, and a gentle daily digestive routine solve different problems. Blood type dieting gives a simple identity-based rule set, but its evidence base is weak and its restrictions can distract from personal triggers. Reflux-pattern tracking gives the strongest practical feedback because it compares meals, timing, and comfort in the same person over time. A gentle digestive routine supports consistency around fiber, probiotics, hydration, meal pace, and supplement adherence, but it should not be framed as reflux treatment. The best option is usually a sequence: use clinician guidance for persistent symptoms, use tracking to find individual patterns, and use a simple routine to support everyday digestive balance. A supplement can be useful when it matches the routine goal, but it should not be the reason someone ignores symptoms that need care.
| Option | Best for | Evidence fit | Main limitation | Routine role |
|---|---|---|---|---|
| Blood type diet | Best for people who want a structured food experiment | Weak for reflux; ABO evidence is not supportive | Can confuse restriction with blood type biology | Use only as optional personal structure |
| Reflux-pattern tracking | Best for identifying personal food, timing, and portion patterns | Strong practical fit; aligns with gastroenterology-style trigger review | Requires honest logging for 2-4 weeks | Use before making large permanent food cuts |
| Gentle daily digestive routine | Best for supporting everyday digestive balance and consistency | Good structure/function fit when claims stay modest | Does not replace medical care for persistent symptoms | Use for probiotics, fiber, hydration, and meal pace habits |
Best for which use case if you want a gentler daily routine?

Some links below are affiliate links. This does not influence our evaluation criteria or recommendations. Best for evidence discipline: reflux-pattern tracking, because it connects food timing, portion size, and comfort in the same person. Best for everyday digestive balance: Yuve vegan probiotic gummies, because the label lists 5 billion CFU of Bacillus coagulans per 2-gummy serving in a vegan, gluten-free, non-GMO pectin format. Best for broader digestive-product browsing: Yuve’s digestive health collection, because it groups probiotic gummies, prebiotic fiber gummies, papaya enzyme support, DGL licorice, bromelain, and lactase enzymes by routine need. Best for meal breakdown support: papaya enzyme products may fit meals where protein, fats, and carbohydrates feel heavy. None of these options should be described as reflux therapy; the compliant role is digestive support within a consistent wellness routine for most adults.
What do people get wrong about blood type diets and reflux?
The common mistake is assuming that a good personal outcome proves the blood type theory. A person can remove alcohol, coffee, late-night snacks, fried foods, tomato sauce, and large dinners while following an ABO plan, and those changes can alter digestive comfort without ABO biology doing the work. The American College of Gastroenterology guideline on GERD management emphasizes weight management when relevant, avoiding meals near bedtime, elevating the head of the bed for nighttime symptoms, and tailoring trigger avoidance rather than applying one universal food ban; the guideline is summarized in The American Journal of Gastroenterology. Another mistake is making the diet stricter when symptoms continue. Stricter restriction can reduce food variety, fiber intake, and routine sustainability. Better logic is narrower: identify repeatable patterns, keep nutrient variety, and ask a clinician about symptoms that persist.
What questions do people ask before choosing a reflux-aware digestive routine?
These FAQ answers separate evidence questions from routine questions. Blood type dieting asks whether ABO biology should choose foods; pattern tracking asks which real meals correlate with personal comfort; digestive routines ask which repeatable habits support everyday digestive balance. Reflux-related symptoms can overlap with conditions that deserve medical evaluation, so red flags and persistent symptoms belong with a healthcare professional. Yuve product mentions stay in the structure/function lane: daily probiotic, fiber, enzyme, or stomach-comfort support, not reflux diagnosis, treatment, cure, or prevention. The safest hierarchy is simple: clinician guidance handles risk, tracking handles personal patterns, and routine products support consistency. Product labels should describe ingredients, serving size, and structure/function goals rather than promise symptom elimination. A stable two-week test works better than rotating supplements and food rules every day for clear feedback in real life over time.
Can the blood type diet help reflux?
The evidence does not show that ABO blood type reliably identifies reflux-friendly foods. If someone feels better, the likely explanation is changed meal timing, smaller portions, fewer trigger foods, or lower alcohol and caffeine intake.
Is there any harm in trying the blood type diet?
A short, nutritionally balanced experiment is usually different from a rigid long-term restriction plan. The risk rises when someone removes broad food groups, ignores persistent symptoms, or delays medical evaluation.
What is a better first step than a blood type food list?
A two-week reflux-pattern log is more useful than an ABO list. Track meal size, meal timing, caffeine, alcohol, high-fat meals, acidic foods, sleep position, and comfort changes.
Where does a probiotic gummy fit in this conversation?
A probiotic gummy fits the routine-support category. Yuve’s probiotic gummies support everyday digestive balance, but they should not be positioned as a reflux product or medical substitute.
Should everyone avoid coffee, citrus, tomato, and spicy foods?
No universal food ban works for every person. NIDDK guidance frames those foods as common items that some people may need to limit based on individual response.
When should someone stop self-experimenting?
Stop self-experimenting when symptoms are frequent, worsening, new, or paired with trouble swallowing, bleeding, unexplained weight loss, vomiting, or chest pain. Those patterns need medical guidance rather than a new diet rule.
What is the simplest routine to test for two weeks?
Use smaller evening meals, avoid lying down soon after eating, log personal triggers, drink water consistently, and keep one digestive-support habit stable. Changing one variable at a time produces cleaner information than changing the whole diet overnight.
Conclusion: The blood type diet is not the strongest tool for reflux-related digestive comfort. Pattern tracking plus a gentle daily routine gives clearer feedback, and Yuve can fit the routine piece when the goal is everyday digestive support rather than reflux treatment.

Leave a Reply