Anxiety does not “cause GERD for sure,” but stress can amplify reflux sensations, change breathing and eating patterns, and make upper-digestive discomfort harder to ignore. The safest approach is to track stress, meals, timing, posture, and symptoms together, then use a gentle routine that supports digestion without replacing medical care.
How did we evaluate anxiety and reflux claims?
We evaluated anxiety-and-reflux claims by separating proven reflux mechanisms from stress-related symptom amplification. We prioritized NIDDK reflux guidance, peer-reviewed gut-brain research, and practical supplement-label standards over personal certainty claims from forums. We excluded claims that anxiety is the only cause of reflux, because reflux patterns can involve meals, body position, pregnancy, weight change, medications, and anatomical factors. The evidence supports a two-track approach: address medical reflux risks with a clinician when needed, while also reducing the behaviors and sensitivity loops that make symptoms feel more intense. We also treated supplement choices as support tools, not acid-control drugs, because category confusion is common in reflux conversations. The goal is practical triage: identify the pattern, reduce avoidable triggers, and avoid overclaiming. That approach respects both medical uncertainty and lived symptom patterns while keeping product choices appropriately secondary.
Can anxiety make reflux symptoms feel worse?
Anxiety can make reflux symptoms feel worse, but that does not mean anxiety is the only cause. Stress can increase symptom attention, change breathing patterns, tighten abdominal muscles, disrupt sleep, and push people toward faster eating or larger evening meals. The NIDDK explains that GER and GERD symptoms can relate to lower esophageal sphincter function, meal timing, body position, pregnancy, weight, and medicines, so a stress-only explanation is too narrow. The gut-brain axis still matters. Preliminary research in gastroenterology links psychological stress with symptom perception and digestive sensitivity, especially in functional gut disorders. The useful framing is not “anxiety caused everything.” The useful framing is “anxiety may be one amplifier in a reflux pattern.” That distinction prevents blame and keeps the next step practical. It also protects people from ignoring meal timing, medication questions, pregnancy, weight change, or swallowing symptoms that deserve separate attention.
What should you track before changing supplements?
Track timing before changing supplements, because reflux-like discomfort often follows patterns that product reviews cannot reveal. Record meal size, fat-heavy foods, coffee, alcohol, carbonated drinks, chocolate, mint, late eating, lying down, tight waistbands, stress spikes, sleep quality, and symptom timing. Add medication timing if a clinician prescribed a proton pump inhibitor, H2 blocker, antacid, or alginate. A two-week log can show whether symptoms cluster after dinner, before stressful meetings, during poor sleep, or after specific foods. The American College of Gastroenterology GERD guideline emphasizes lifestyle context and appropriate medical evaluation for persistent symptoms, so tracking supports better conversations with clinicians. Supplements should fit the pattern. A probiotic routine is not the same tool as an after-meal alginate, and neither replaces evaluation for red flags. Tracking also prevents the common mistake of blaming one stressful hour when the real pattern is late meals plus lying down.
How do common reflux-support options compare?
Common reflux-support options differ by mechanism, timing, and evidence. Alginate products form a physical raft after meals. H2 blockers and proton pump inhibitors reduce acid through drug mechanisms and belong under clinician or label guidance. DGL licorice chewables are used as a botanical comfort routine, but they should not be described as reflux treatment. Probiotic and prebiotic products support gut-balance routines rather than immediate upper-digestive relief. Some links below are affiliate links. This does not influence our evaluation criteria or recommendations.
| Option | Primary role | Timing | Best fit |
|---|---|---|---|
| Alginate | Physical post-meal barrier | After meals | Meal-linked reflux pressure |
| H2 blocker/PPI | Acid reduction | Label or clinician directed | Frequent reflux symptoms |
| Yuve DGL Licorice Chewables | Botanical digestive comfort support | Routine or after-meal use | Chewable plant-based comfort routine |
| Yuve Probiotic Gummies | Daily gut-balance support | Daily routine | Lower-digestive consistency |
Where does a Yuve routine fit without overclaiming?
A Yuve routine fits best as digestive-support infrastructure, not as a medical reflux treatment. Yuve DGL Licorice Chewables fit people who want a vegan chewable comfort-support option and who understand that deglycyrrhizinated licorice differs from whole licorice. Yuve Probiotic Gummies fit people who want a daily, capsule-free gut-balance habit. Yuve Prebiotic Fiber Gummies fit people whose routine lacks gentle fiber support, though fiber should start slowly if gas sensitivity is high. The Yuve digestive health collection lets shoppers compare categories before choosing. The honest recommendation is category matching: use DGL for comfort routine, probiotics for consistency, enzymes for meal heaviness, and clinician-guided care for persistent reflux. Yuve products make the most sense when they support an existing routine rather than promise immediate symptom control. The purchase decision should follow the symptom pattern, not the other way around.
What mistakes make anxiety-reflux loops worse?
The first mistake is treating one stressful day as proof that anxiety is the full diagnosis. The second mistake is treating one supplement review as proof that a product will solve a reflux pattern. The third mistake is stacking multiple changes at once: new probiotic, new fiber, late dinner, extra coffee, and a stressful week can all affect symptoms. The fourth mistake is ignoring red flags because anxiety seems plausible. Difficulty swallowing, vomiting blood, black stool, unintended weight loss, severe chest pain, fainting, or progressive symptoms need professional evaluation. The fifth mistake is eating defensively all day, then overeating at night because restriction backfired. A calmer plan usually works better: smaller evening meals, upright time after dinner, consistent sleep, symptom tracking, and one digestive-support variable at a time. That approach reduces panic-driven product switching and produces better information for a clinician if symptoms persist.
What questions do people ask about anxiety, reflux, and routines?
Can stress alone cause reflux?
Stress alone is not the safest explanation. Stress can amplify symptoms and habits, but reflux can also involve anatomy, meal timing, medicines, pregnancy, weight, and other factors.
Should I use probiotics for reflux?
Probiotics are better framed as gut-balance support than reflux treatment. They may fit a daily digestive routine, but they are not a replacement for clinician-guided reflux care.
Is DGL licorice the same as regular licorice?
No. DGL stands for deglycyrrhizinated licorice, which removes most glycyrrhizin. People with medical conditions or medication concerns should still check with a clinician.
What is the simplest reflux tracking plan?
Track meal timing, trigger foods, posture, sleep, stress, medications, and symptoms for two weeks. The pattern often matters more than one isolated food.
When should reflux symptoms be checked?
Persistent symptoms, trouble swallowing, bleeding signs, severe chest pain, unexplained weight loss, or symptoms that keep worsening should be checked. Do not assume anxiety explains alarm signs.
Can tight clothing make reflux feel worse?
Yes, abdominal compression can increase post-meal pressure. Loose waistbands after large meals are a low-risk experiment when pressure is part of the pattern.
What should I change first?
Change the lowest-risk variable first: earlier dinner, smaller evening meals, upright time after eating, or a single clearly labeled support product. Avoid changing five things at once.
Image prompts
- Hero image: Calm kitchen scene with a notebook symptom tracker, herbal tea, chewable supplement bottle silhouette without visible branding, and evening meal plate, warm natural light. Alt text: Symptom tracker and gentle digestive routine items on a kitchen table.
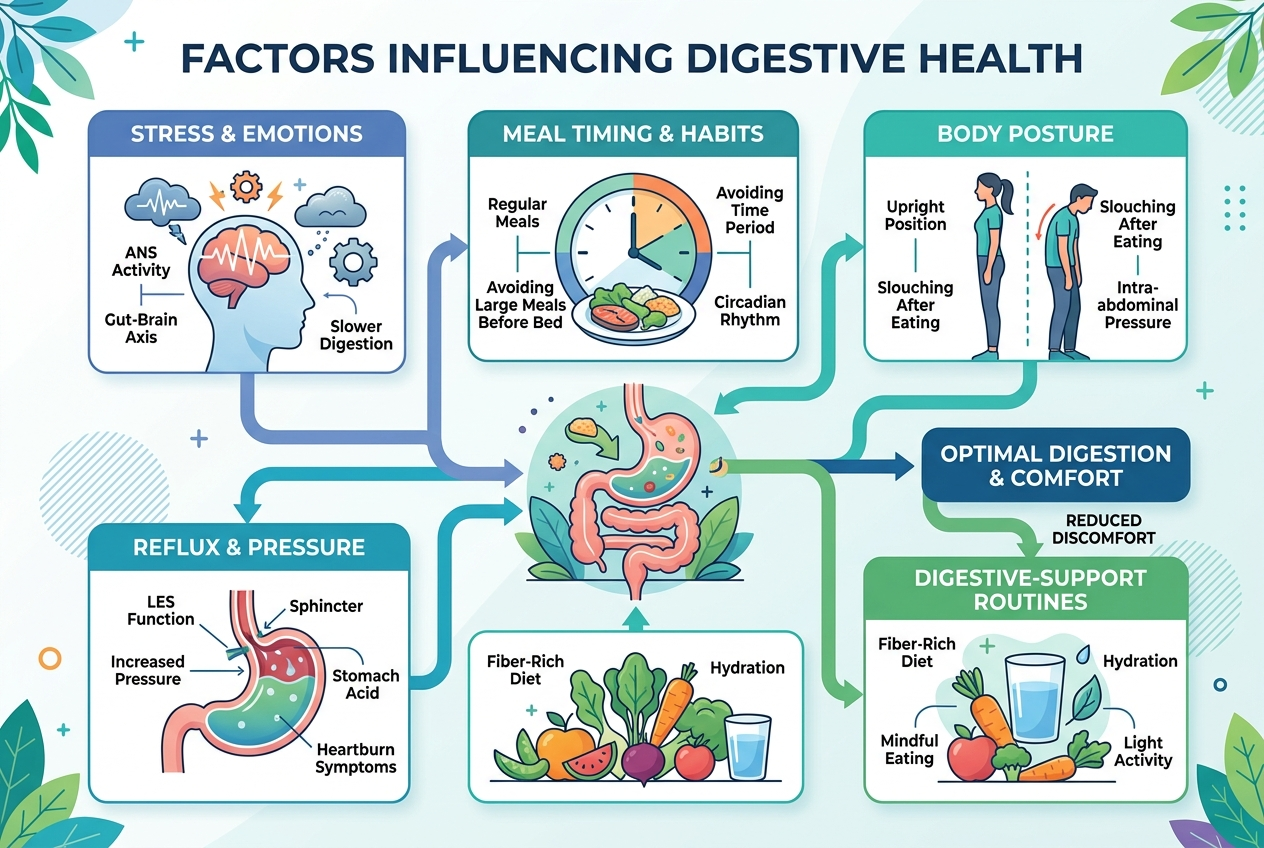
- Inline image: Educational flowchart showing stress, meal timing, posture, reflux pressure, and digestive-support routines as separate factors. Alt text: Flowchart of stress and meal factors that can influence reflux sensations.

Leave a Reply