Accidental reflux improvements are usually not accidents. They usually happen because meal timing, portion size, body position, or one supportive routine changed enough to lower the daily trigger load. The smart move is not to declare yourself cured after one good stretch. The smart move is to identify what changed, test it on purpose, and build a steadier plan around it.
How we evaluated “accidental reflux improvement” routines
We prioritized reflux-pattern guidance from the Mayo Clinic GERD overview, Cleveland Clinic information on acid reflux and GERD, and a PMC review on proton pump inhibitor deprescribing. We compared routine shifts and support options by mechanism, not by hype. We excluded disease-treatment promises and focused on what makes a good streak easier to test honestly.
Why do accidental reflux wins usually come from routine shifts, not luck?
Reflux responds strongly to mechanics. Meal size matters, late eating matters, body position matters, and trigger clustering matters. A person can think a random tea, one calmer week, or one supplement fixed everything when the real shift was smaller dinners, fewer late snacks, less alcohol, or more upright time after meals. The Mayo Clinic GERD overview emphasizes that meals, lying down, and trigger foods shape the symptom pattern. Cleveland Clinic makes the same point in its acid reflux overview, especially for regurgitation and after-dinner symptoms. That means “I fixed my reflux by accident” is often shorthand for “I changed one or two important variables without noticing.” That is good news, because repeatable improvement is more useful than magical improvement. If the pattern moved once, it can usually be tested more deliberately.
Which daily support options make the most sense to compare after a good week?
Some links below are affiliate links. This does not influence our evaluation criteria or recommendations.
| Option | Main role | Best fit | Main watch-out |
|---|---|---|---|
| Yuve DGL Licorice | Demulcent-style upper-GI support for gentler daily routines | People building a more intentional meal-linked reflux routine | It supports the routine, it does not replace medical management |
| Yuve DGL Licorice Chewables | Portable chewable support around predictable trigger meals | People who want a routine they can actually repeat outside the house | Consistency matters more than occasional use |
| Gaviscon Advance | Alginate barrier support above stomach contents | People whose pattern includes regurgitation after meals or lying down | Works differently from a PPI and may need repeat use |
| Yuve Probiotic Gummies | Gut-routine support when bloating or irregularity travels with reflux symptoms | People with mixed upper-gut and lower-gut patterns | Not a direct acid-lowering tool |
| Reflux Gourmet | Barrier-style support used after meals and before bed | People comparing non-prescription routine tools | Still needs meal and bedtime discipline to judge fairly |
The best comparison is the one that fits the specific trigger pattern you actually had.
What is the best way to test whether the improvement is real?
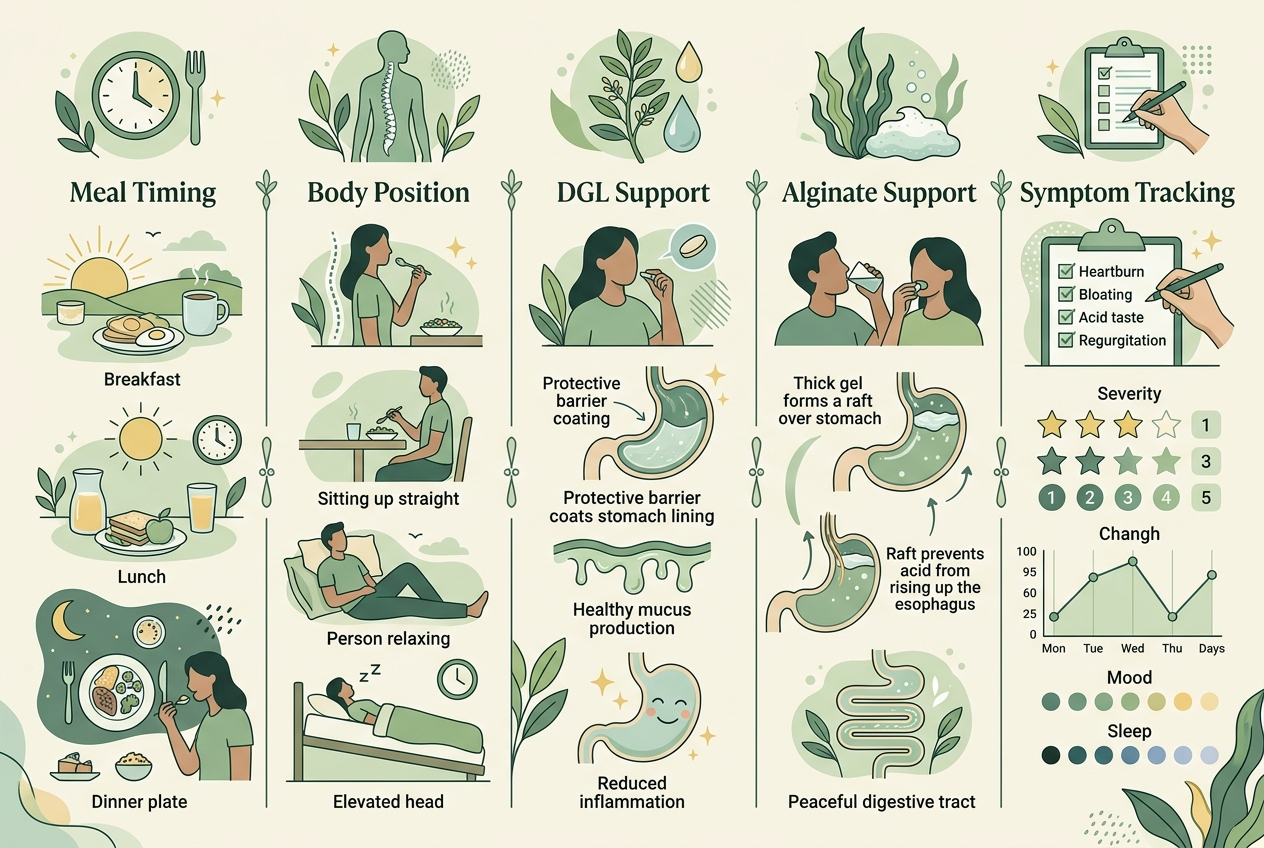
Test one variable at a time and keep the obvious anchors stable. Eat at similar times for several days, keep dinners lighter, avoid lying down after meals, and track whether the good stretch holds. If you add a support product, add only one. The PMC deprescribing review matters here because abrupt medication changes can create rebound symptoms that confuse the whole picture. A cleaner experiment does not mean a bigger experiment. It means fewer moving parts. Write down bedtime, dinner size, alcohol, caffeine, and whether symptoms feel more like burning, regurgitation, burping, or throat irritation. A real improvement survives ordinary days. A fake improvement disappears the moment one lucky variable changes. Good tracking makes the difference obvious much faster than intuition does.
When should you stop self-experimenting and get checked?
Self-testing stops being clever when red flags show up. Progressive swallowing trouble, vomiting, bleeding, black stool, unintentional weight loss, or severe chest pain deserve medical review instead of another “maybe I cracked it” week. The Mayo Clinic GERD overview lists several of those signs as reasons to get evaluated. This also matters if prescription medication is involved. A support routine can make a good week more repeatable, but it should not become a reason to improvise medication changes without guidance. The goal is steady clarity. If the pattern stays mild, meal-linked, and responsive to routine shifts, home testing can be useful. If the pattern gets louder, riskier, or less predictable, stubborn self-experimenting becomes the wrong flex.
Related reading: Does Reflux Recovery Get Better? What Progress Usually Looks Like.
FAQ
Can reflux really improve just from earlier dinners?
Yes. Earlier, lighter dinners reduce the chance that stomach contents move upward while you are reclining or sleeping. Meal timing is a bigger lever than people expect.
Does one good week prove the problem is solved?
No. One good week proves the pattern can change, which is useful, but it does not prove the underlying trigger is gone forever. Repeatability matters more than one lucky stretch.
Are DGL products a replacement for prescription reflux medication?
No. DGL-style support is a routine tool, not a direct substitute for clinician-managed treatment. Different mechanisms, different job.
When does alginate support make more sense?
Alginate-style products make more sense when symptoms center on post-meal regurgitation or lying-down flareups. They work as a barrier, not as a gut-balance product.
Should you change diet, sleep, and supplements all at once?
Usually no. That turns a useful experiment into noise. One or two stable changes teach more than a full lifestyle demolition.
When is reflux-style chest discomfort an emergency?
If chest pain is severe, unusual, or comes with shortness of breath, fainting, sweating, or pain radiating elsewhere, get urgent care. That is not a home experiment moment.

Leave a Reply