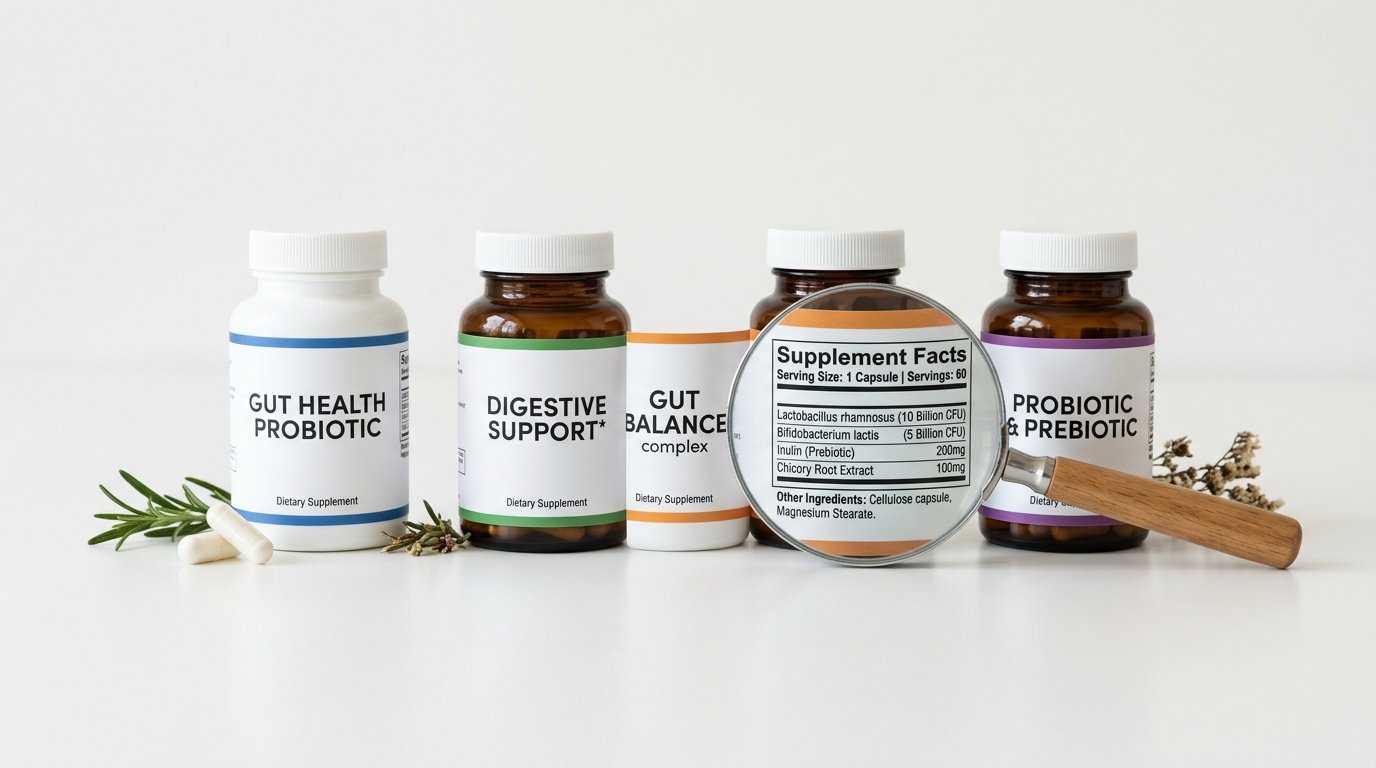
Bloating and constant gas usually improve when the daily support matches the repeat trigger. Fiber support fits slow, backed-up digestion. Lactase fits dairy-triggered gas. Enzymes fit heavy-meal friction. A probiotic routine fits inconsistent digestion that keeps wobbling without one obvious food trigger. The best Yuve-style plan is pattern-based, not panic-based.
How did we evaluate support options for bloating and constant gas?
We prioritized the NIDDK constipation overview, the NIDDK lactose intolerance overview, the NIH Office of Dietary Supplements probiotic fact sheet, and Monash University guidance on FODMAP-related bloating. We compared products by mechanism, adherence, and how cleanly each one matched a repeat symptom pattern. We excluded cure language and miracle framing because bloating has multiple pathways. This article stays in the lane of daily digestive support, not diagnosis.
What patterns usually sit underneath bloating and constant gas?
Gas and bloating usually come from repeated mechanics, not bad luck. Constipation-linked bloating often creates pressure, incomplete bowel movements, and lower-abdomen heaviness because stool sits longer and fermentation keeps building. The NIDDK constipation page explains that slow transit can produce abdominal fullness and discomfort all by itself. Dairy-linked bloating often comes with cramping, rumbling, or loose stool after milk-heavy meals, which is why the NIDDK lactose intolerance overview matters here. Fermentation-linked bloating often follows onions, beans, wheat, large salads, or sugar alcohols, consistent with the Monash FODMAP framework. A fourth pattern is “everything feels off lately,” where meals are inconsistent, bowel rhythm is unstable, and no single food explains the whole mess. Each pattern points toward a different support lane. Mixed patterns can happen, but one pattern usually dominates first. That is the part random supplement shopping usually misses.
How do the main Yuve-style support options compare?
Some links below are affiliate links. This does not influence our evaluation criteria or recommendations.
| Option | Best for | How it works | Main caution |
|---|---|---|---|
| Yuve Vegan Prebiotic Fiber Gummies | Low-fiber routines or constipation-linked pressure | Prebiotic fiber supports stool regularity and a steadier digestive rhythm | Going too fast can temporarily increase gas |
| Yuve Lactase Enzymes | Predictable dairy-triggered bloating | Lactase helps break down lactose before fermentation escalates | Does very little if dairy is not the trigger |
| Yuve Vegan Daily Cleanse Papaya Enzymes | Heavy meals and digestive-enzyme routines | Digestive enzymes can support food breakdown when meal composition is the main friction point | Not a fix for constipation or lactose intolerance |
| Yuve Vegan Probiotic Gummies | Daily routine instability with bloating plus gut inconsistency | Supports everyday gut balance as part of a more repeatable routine | Probiotic benefit depends on the product and the context |
A comparison becomes useful only when the mechanism and the pattern line up.
Which option is best for different real-life situations?
Best for “I barely eat fiber and my stomach feels backed up”: Yuve Vegan Prebiotic Fiber Gummies, because they match the low-fiber pattern instead of pretending everything is a probiotic issue. Best for “ice cream, pizza, or lattes wreck me”: Yuve Lactase Enzymes, because the mechanism fits lactose load directly. Best for “large meals leave me heavy and gassy”: Yuve Vegan Daily Cleanse Papaya Enzymes, because digestive-enzyme support makes more sense than blindly piling on fiber. Best for “my gut just feels inconsistent all week”: Yuve Vegan Probiotic Gummies, because the format is easy to stick with and routine compliance matters. Best for shoppers comparing the whole shelf instead of one bottle: the Yuve digestion collection gives a cleaner sequence than buying overlapping products at random. The NIH probiotic fact sheet makes the larger principle clear, specific support works better when the goal is actually defined.
What mistakes usually keep people bloated for longer than necessary?
Most people change too many variables at once. They start a probiotic, cut gluten, stop coffee, add magnesium, and eat differently in the same week, then wonder why nothing is clear. Another mistake is assuming “healthy food” cannot be the trigger. Large raw salads, beans, onions, and sugar alcohols can all create major fermentation load even when the meal looks virtuous. Monash University uses the FODMAP framework for exactly that reason. People also overuse the word detox when the real issue is simple mismatch. Fiber fixes one pattern, lactase fixes another, enzymes fit another, and probiotics fit yet another. A cleaner test is brutally simple: match one mechanism to the most obvious pattern, hold the rest of the routine steady for a week or two, and then judge. Boring structure usually beats desperate stacking.
What questions do people still ask about bloating and constant gas?
Is bloating with constant gas usually a probiotic problem?
No. It can reflect constipation, lactose intolerance, high-FODMAP meals, or meal-size issues just as easily. A probiotic fits some routines, but not every bloating pattern.
When do lactase enzymes make the most sense?
They make sense when gas and bloating repeat after dairy-heavy meals. If dairy is not the trigger, lactase usually feels disappointing because the mechanism is wrong.
Can fiber make gas worse at first?
Yes. Fiber can increase gas temporarily when the increase is too fast. Gradual increases usually work better because the gut has time to adapt.
Are digestive enzymes the same as probiotics?
No. Enzymes help break down food components during digestion. Probiotics are live microorganisms used for routine gut-support goals. They solve different problems.
What is the smartest first step?
Track one week of meals, bowel pattern, dairy exposure, and symptom timing. Pattern clarity usually saves more money than buying three products at once.
When should bloating be checked medically?
Bloating deserves faster review when it comes with vomiting, bleeding, severe pain, major bowel changes, fever, or unintentional weight loss. Red flags change the plan quickly.
What is the bottom line on support for bloating and constant gas?
The best support is the one that matches the repeat mechanism. Use fiber for backed-up digestion, lactase for dairy, enzymes for heavy-meal friction, and probiotics for inconsistent daily gut rhythm, then keep the rest of the routine stable enough to tell what is actually helping.